Understanding & Addressing Resistance to Change in Healthcare Organizations | Best Change Management Guide

Breaking the Mold: A Guide to Overcoming Barriers in Healthcare and Nursing
Welcome to a transformative journey in healthcare and nursing—a guide where we delve into the intricate dance of change. Navigating the ever-evolving landscape of healthcare is akin to orchestrating a symphony, where every note resonates with the potential to enhance patient care, elevate operational efficiency, and elevate the overall healthcare experience.
In this guide, we embark on a mission to conquer the barriers that often stand between innovative ideas and their seamless integration into the fabric of healthcare organizations.
Change is not merely an event; it’s a process that involves individuals, teams, and entire cultures.
Whether you’re a dedicated healthcare professional seeking to implement new procedures or a change manager navigating the complex dynamics of transformation, this guide is your companion in understanding, addressing, and triumphing over the challenges that change inevitably brings.
Join us as we explore the unique nuances of resistance—be it from individuals adjusting to new healthcare procedures, cohesive departments grappling with shifts, or visionary leaders steering the organizational ship. We’ll unravel the intricacies of change management, offering insights into tailored strategies that resonate with the heartbeat of healthcare.
Excited to discover the road ahead? We’ve crafted a succinct summary for you. Get ready to explore the intricacies of overcoming barriers to change in healthcare and nursing, reassured by the knowledge that we’re here to guide you through this insightful journey.
Quick Summary
Breaking Through: Addressing Resistance in Health Care Change Initiatives
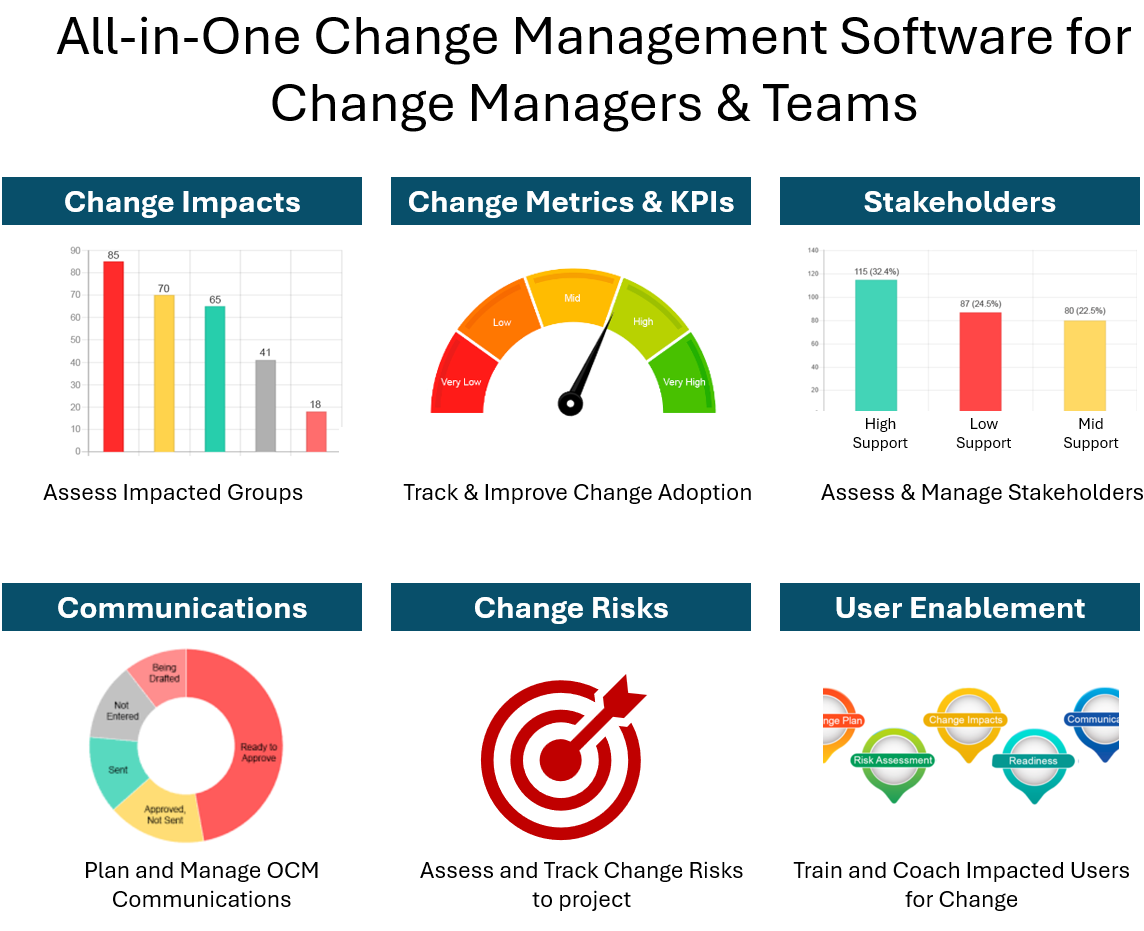
There are various sources of resistance to changes in healthcare with highlights to six key areas where barriers to change may arise. These areas include:
- Individuals: People undergoing changes in healthcare procedures may experience emotions such as anxiety, anger, or confusion. Their resistance can become a barrier to change.
- Departments/Groups: Resistance can come from groups within the healthcare organization, like specific floors or groups of physicians. Strong group identity and culture may lead to collective opposition, especially if key leaders within the group are against the change.
- Organization/Leadership: Unrealistic expectations from top management, such as unrealistic timelines or inadequate allocation of funds, can create barriers to change. If these aspects are not realistic, the change project may be set up to fail.
- Change Managers: Those responsible for managing change within healthcare organizations can inadvertently become barriers. Lack of a well-defined change management strategy and insufficient communication during the change process can lead to problems.
- Technology: The tools needed for healthcare changes, such as new technologies, may have their own issues. Difficulties in using the technology or unexpected glitches can stall the change project.
- 3rd Party Support: Some healthcare changes rely on third-party support, such as vendors providing training for new equipment. If these external partners fall short in support or if there’s miscommunication about expectations, it can create barriers to implementing changes in healthcare.
Proactive awareness of these potential barriers is fundamental for overcoming resistance and ensuring successful implementation of healthcare changes.
Innovation Hurdles: Understanding and Resolving Change Barriers in Healthcare
The passage explores barriers to change in healthcare organizations and provides insights into overcoming them. It emphasizes the importance of a competent change management team and the use of best practices, including employing change models and methodologies. The text identifies and elaborates on six key areas of resistance:
- Individuals: Discusses the emotional aspects of individual resistance to change in healthcare, citing the Bridge’s Transition Model. It highlights the importance of addressing emotions, fears of job loss, and ensuring proper training for new processes.
- Departments/Groups: Examines group dynamics and the challenges of overcoming resistance within a collective. Emphasizes the identification of group leaders who can support the change and suggests tools like impact assessments and leadership coaching.
- Organization/Leadership: Discusses barriers originating from leadership, such as changing project missions mid-stream, inadequate budgeting, and unrealistic expectations. Solutions include effective communication, project assessments, and the use of change models.
- Change Managers: Explores potential barriers arising from change managers, such as lack of planning and attempting shortcuts. Advocates for change models, comprehensive change management strategies, and the use of an all-in-one change management tool.
- Technology: Highlights technology-related barriers that can stall change projects, emphasizing the need for flexibility, thorough testing, and collaboration with IT teams to address issues promptly.
- 3rd Party Support: Examines challenges related to third-party vendors and suggests clear communication, setting expectations, and including vendors in project planning as solutions.
The passage underscores the significance of proactive strategies, including resistance management tools, change models, training plans, and clear communication, to successfully navigate and implement change in healthcare organizations.

Overcoming Obstacles: Strategies for Addressing Physician Resistance to Change
Physicians play a critical role in healthcare when it comes to decision-making, and acknowledging that their support is vital for implementing changes in procedures or policies. However, due to the significance of their responsibilities, getting physicians on board can be challenging.
With dedicated efforts and allocating a part of the change management team to help address their resistance changes in healthcare procedures the chances of changing a physician’s culture greatly increases.
Here are some of the key reasons for physician resistance to change:
- Established Habits: Physicians develop their own ways of doing things over time, shaped by their interactions with patients, knowledge, and experience. Even small changes that affect these habits can lead to resistance among physicians to adopt new nursing or healthcare procedures.
- Shared Culture: Physicians share a unique culture with one another. Given the immense responsibilities they bear daily, they tend to form close bonds with colleagues who can truly understand their experiences. This shared culture adds complexity when addressing resistance to change within the group.
- Group Resistance: Dealing with resistance from a group, such as physicians, is more challenging than dealing with individual resistance. The shared culture and dynamics among physicians contribute to this complexity.
- Decision-Making Authority: Physicians are typically in charge, making critical decisions about patient care, medications, discharges, and more. When accustomed to being in control, being told to change can trigger immediate resistance to adopting new nursing or healthcare procedures.
- Influence on Other Groups: The resistance of physicians to change can create barriers for other groups within the healthcare organization. If physicians resist, other groups might question the necessity of changing and wonder why they should bother if the leaders aren’t changing.
There are many unique challenges posed by physicians’ resistance to change in healthcare and its important to understanding their habits, culture, and leadership roles to successfully implement changes across the organization.
Physician Culture Shift: Strategies to Navigate Resistance in Healthcare
Changing a physician’s culture is no easy feat but there are several strategies for overcoming resistance to change these include:
- Logical Explanation with Data: Acknowledge physicians’ data-driven nature and problem-solving mindset by logically explaining the benefits of the change. Use data to support how the change will positively impact the organization, patients, and physicians themselves.
- Respect for Their Time: Recognize the time constraints physicians face and tailor training processes to be flexible and time-sensitive. For instance, offering audio training that can be accessed during commutes helps accommodate their busy schedules.
- Enlist Key Physicians as Change Agents: Overcome the challenge of being an outsider in the physician culture by involving well-respected physicians in the change process. Utilize these key physicians as change agents and champions to effectively communicate and drive the change within the community.
- Utilize Change Management Toolkit: Apply standard change management tools, such as a resistance assessment and communication plan, to identify and address emotional resistance to changes in healthcare organizations. Despite differences between physician and other groups, core reasons for resistance often share common emotional elements.
Its important to recognize how vital tailoring change management strategies is when analyzing the unique characteristics of the physician culture, addressing their data-driven mindset, time constraints, and the need for internal influencers in the change process.
Detailed Deep Dive
Healthcare is an industry that sees a significant amount of change. Changes in healthcare facilities can be due to factors like mergers, new medical discoveries, cost-cutting measures, or new regulatory guidelines.
The nature of healthcare means it’s always changing and evolving to better meet patient needs while balancing that with staffing, budgetary, and technological demands.
But just because change may happen more in the healthcare industry than some other fields, doesn’t mean it’s not without its challenges.
Just because a process or system needs to change, doesn’t mean making that change happen is going to be easy.
In fact, there are many barriers to change in healthcare organizations that cause projects to stall, completely fail, or fall short of their objectives. These barriers can be coming from people, leadership, technology, or any number of other areas.

A Healthcare Change Manager Addressing Healthcare Stakeholders
To overcome these barriers to implementing change in healthcare facilities, you must first identify where the resistance is coming from. After that, you need to implement procedures to address the resistance to change in nursing or healthcare so you can move past it and drive the change forward.
What This Guide Provides to You and Anyone Interested in Resolving Resistance to Change in Healthcare & Physician Practices
In this article, we’re going to take a look at the key categories that barriers to implementing change in nursing or healthcare fall into. We’ll look separately at resistance to change in nursing practice and why it can be so hard for physicians to adopt change.
In each category of resistance to culture change in healthcare, we’ll see what the main resistance factors are and ways to address them using change management best practices.
We’ll explore why people resist change in the healthcare sector, how to move them to an accepting and supporting state, and go through some of the barriers that organizations put up that impede changes in healthcare facilities.
While there can be many barriers to change in nursing and healthcare, there is also plenty of change methodology out there to help health professionals move past obstacles and implement much-needed changes successfully.
See Also: Applying Best Change Management in Healthcare | All You Need to Know
Do you have questions on the challenges to implementing change in healthcare or the reasons for resistance to change in healthcare like found in this article. We’d love to hear from you, click here to contact us.
Overview | Barriers to Change in Health Care?
Let’s first discuss the general categories of barriers to change in healthcare organizations. Then we’ll go into detail about the types of resistance in each one and how to address it.
Resistance to recent changes in healthcare can come at you from different areas all at the same time. This includes from people undergoing the change and from things outside your control, like technology glitches.
Being aware of where to proactively look for those barriers can help you in overcoming resistance to change in healthcare processes and be more prepared to resolve and move past resistance.
Here are the six key areas where you’ll encounter resistance to changes in health care processes and procedures.
Individuals
Change isn’t just something that happens to an organization; it’s something that also happens to each individual that has to go through changes in healthcare procedures.
The way a person has always done something is going to change, and they can feel anxious, angry, confused, and many other emotions that can turn into barriers to change in healthcare organizations.
Departments/Groups
Resistance to change in nursing and healthcare can also come from a group. It might be the pediatrics floor or your surgical physicians. When you have a strong group identity and culture, it can cause people to band together against a change.
Sometimes just a few key leaders in a tight-knit group that are against a change can cause significant resistance to change in healthcare organizations.
Organization/Leadership
If the people at the top, i.e., the ones allocating funds for a change or setting a timeline, aren’t being realistic about the needs of the change project, it can cause several barriers to change in nursing and healthcare processes that set it up to fail before it even begins.
Change Managers
Those managing a procedure or culture change in healthcare organizations can get in their own way and become a barrier themselves. Things like lack of a change management strategy and insufficient communication during the change can lead to problems that turn into barriers to change in healthcare organizations.
Technology
The tools that you need to facilitate the change or that you are moving to as part of your recent changes in healthcare processes can have their own issues that cause your project to stall. Users having difficulty using the technology to manage your change project is another one of the barriers to changes in health care procedures.
3rd Party Support
Some changes in healthcare organizations will rely on third-party support. For example, if you are implementing a new telehealth robot in your hospital, you may depend upon the manufacturer to send a training team to show your maintenance staff how to service it.
If any third-party vendors fall short on their support or if there is miscommunication about expectations, this can cause barriers to implementing change in nursing and health initiatives.
Don’t Miss: The Best Practices for Changing Organizational Culture in Healthcare
Got questions like “How to overcome resistance to change in healthcare?” or “What are the barriers to implementing change in healthcare?”. Drop us a message and let us know.
Detail & Solutions | Barriers to Change in Healthcare Organizations?
Being able to identify and overcome resistance to change in nursing practice and healthcare facilities is the mark of a good change management team.
Using change management best practices, which include using a change model and methodology to guide your change project, helps tremendously in overcoming resistance to change in healthcare.
As we go into more detail below on the categories of barriers to implementing change in healthcare facilities, we’ll discuss the types of barriers you’ll encounter in each. We’ll also talk about some of the change management tools and methods you can use to resolve resistance to change in nursing and healthcare.
Change Barrier: Individuals
To understand why people resist change it helps to a look at the Bridge’s Transition Model, which puts changes in health care processes into three phases.
The first phase is called “Ending,” which means the individual is losing something and has to let go of a comfortable process they may have used for years. This can lead to feelings of confusion, denial, frustration, and more. All of which can cause resistance to change in healthcare organizations.
The most successful change models used in nursing and healthcare are ones that emphasize the human aspect of changes in health care processes to help change managers identify and respond to individual resistance.
Individual resistance to change in healthcare organizations isn’t always coming from the same emotions. Some people may be scared about losing their job, while others might have been through too many “bad” changes, that they don’t see the point in another one.
The other types of individual barriers to change in nursing and healthcare has to do with skills. Have people been trained properly? Given enough time to master the new processes?
If individual skills aren’t ready for the change and employees don’t yet have the knowledge or ability to sustain the change, this is another serious problem.
Solutions:
When dealing with a culture change in healthcare organizations that causes individual barriers to crop up, you can employ some of the following solutions.
- Use a resistance management tool that will help you proactively and reactively address resistance to change in nursing practice and healthcare initiatives.
- Employ a change management model, such as ADKAR, that identifies the stages employees must be guided through during changes in healthcare organizations.
- Create a training plan that will help ensure each individual is given a chance to become proficient in the new process before your go-live date.
Departments/Groups
When you’re dealing with why people resist change as individuals, it’s a different dynamic than dealing with a group. It’s often harder to break through group barriers to change in healthcare organizations.
People that don’t have an individual resistance to recent changes in healthcare processes may not want to go against their group, and so will side with the group against the change.
The key here is to identify leaders and individuals in the group that you can get on your side to help facilitate the change and address barriers to implementing change in nursing or healthcare within their group.
Understanding the group culture and dynamics is also very important. Later in this article, we’ll discuss nurse and physician resistance to change in particular.
Solutions:
Tools to help with overcoming resistance to change in healthcare coming from departments are groups are:
- Use an impact assessment tool to help you identify the severity of the impact of the change to various groups within your organization.
- Leadership coaching can help leaders and managers of a group better understand their part in facilitating the change initiative.
- Recruiting a group of employees from different departments for a Change Champions Network can help you communicate the importance of change on the ground level.
Organization/Leadership
The people “at the top” can cause several barriers to implementing change in healthcare, which can impact everything from the resources you have to your timeline.
Changes in healthcare organizations are most successful when leadership is fully on board to support the change and understands the things that need to be accomplished to ensure it’s done right and produces the desired results.
Some of the barriers to change in healthcare projects that you can encounter at the organization/leadership level include:
- Changing the project mission mid-stream
- Not budgeting enough to support a successful change initiative
- Supporting the change on paper, but not in voice or actions
- Having unrealistic expectations about the project timeline
Solutions:
Communicating the project mission, the problem it’s designed to solve, and how it is going to benefit the organization helps you get past the reason why people resist change at the leadership level.
Leadership also needs to understand how vital their support is for the process or culture change in healthcare to be accomplished and meet desired outcomes.
- Do a project assessment to present to leadership, so they fully understand project parameters, milestones, timeline, solution, etc.
Use a change model and proven change approach that helps dispel resistance to change in nursing or healthcare initiatives by leadership.
Change Managers
Some of the barriers to change in nursing or healthcare procedures coming from change managers include lack of planning, not enlisting help from leaders and change champions, and trying to take shortcuts.
The change project is on the shoulders of the change management team, and to be successful takes understanding change management methodologies and both the individual and organizational sides of change.
Solutions:
Change models are invaluable when it comes to facilitating process or culture change in healthcare and driving a change project forward from planning to implementation to completion successfully and sustaining that change.
Here are some of the safety nets you can put in place to avoid becoming a barrier to the project:
- Take the time to learn and understand change models and change management training so you’ll have a base of knowledge to start from.
- Create a detailed change management strategy ahead of time, so you’ll have a roadmap to guide you and your team through the process.
- Use of an All-in-One Change Management Tool can help you keep track of all the different areas of your change project and ensure nothing falls between the cracks.
Technology
Technology problems that cause your change project to stall or interfere with parts of your initiative can be significant barriers to change in healthcare organizations.
Unlike individual or group resistance to change in healthcare procedures, you can’t always address a technology issue directly and may have to wait on a third-party to help.
Technology barriers to changes in health care facilities can include things like users having trouble logging into a webinar service you’re using for training or having difficulty with a new digital tool that staff is learning for the change.
Solutions:
Addressing technology-related barriers to implementing change in nursing or healthcare initiatives requires being flexible and prepared for anything.
- When technology is involved, have a “plan B,” such as a second webinar platform to use, or an alternate cloud messaging tool for communication.
- Test tools thoroughly prior to introducing them to your users during the change project. It’s a good idea to get help from your Change Champions Network for this.
- Develop a relationship with an IT partner or your internal IT team that you can go to for help to get through technology barriers to implementing change in healthcare.
3rd Party Support
If you’re working with third-party vendors, such as a change management consultant or equipment or pharmaceutical representative, this can also be a barrier to your change project.
The more balls you have moving in the air, the more difficult coordination can be. But if you stick to your change strategy and ensure your vendors know what’s expected of them, this can help in overcoming resistance to change in healthcare from third parties.
Solutions:
Communication is key when it comes to vendor management, so treat them as a member of your change team and communicate with third parties accordingly.
- Set clear expectations of the type of support you need for your project before contracting their services.
- Include third party vendors in on your project planning assessment, change management roadmap, and the role they’ll play in driving the change.
- If possible, have another replacement vendor in mind should you not get the support you need for your change project.
Related: Best Guide for Improving Healthcare Leadership in Healthcare & Social Care
Are you looking answers to questions like “What are the barriers to change management in healthcare?” or “Why are nurses resistance to change?” Send us a message with your questions or comments.
Barriers to Implementing Change in Nursing?
Next, we’re going to go over two distinct groups that can cause resistance to change in nursing and healthcare initiatives in different ways. Nurses and physicians. We’ll begin with nurses.

Nurses are one of the most impacted groups when it comes to implementing changes in healthcare facilities. This is because they tend to be the glue that holds everything together in many healthcare organizations.
They interact directly with many other groups, such as patients, physicians, laboratory technicians, billing, etc.
Because Nurses are such an integral part of healthcare facilities, it means they can also cause major resistance to change in healthcare organizations. Sometimes this resistance is unintentional, such as they are just too busy to learn new procedures.
Other times why people resist change in the nursing group is because they haven’t been consulted about the change and feel it doesn’t take their point of view into consideration.
Common causes of resistance to change in nursing practice groups include:
- Being already overwhelmed by current procedures
- Lack of knowledge about how the change will benefit them
- Too busy to have any interest in the change project
- Negative experience with a past change project
- Unwilling to learn the new behaviors
- Afraid they won’t be able to adopt the new skills
Physicians and Change?
In these next few sections, we’ll go through one of the groups that can have the biggest resistance to change in healthcare organizations – physicians.
Because so much of the healthcare process is driven by the life and death decisions made by physicians, getting them on board with changes in healthcare procedures or policies is vital; however, it can also be challenging.
Those managing changes in health care organizations may even want to dedicate part of their change management team just to coordinating with physicians and addressing their resistance to any recent changes in healthcare procedures.
The reason why the rest of your groups within a healthcare organization resist change may be somewhat different than why people resist change when it comes to physicians.
Popular Article: Top Healthcare Consulting Firms | Ranking & Reviews
Are you looking for more information on questions like: “What are the biggest challenges to implementing change in healthcare?” or “What are the main reasons for resistance to change in healthcare?” Send a message to our change management team.
Physician Resistance to Change
Why are physicians known to be resistant to changes in healthcare organizations? Over time, many have established their own habits and ways of doing things based upon a combination of patient interaction, knowledge, and experience.
Even if a change only slightly impacts one of those habits, it can still cause resistance to a change in nursing or healthcare procedures by physicians.
In addition to their own habits, physicians also have a culture with other physicians. It’s not uncommon for people that have so much responsibility placed on their shoulders on a daily basis to have a close bond with the few others that can completely understand what they go through.
As we mentioned earlier, addressing group resistance to change in healthcare organizations is more complicated than addressing individual resistance, and the same is true with the physician culture and group resistance to changes in healthcare organizations.
One also needs to understand that physicians are usually the ones calling the shots. People are asking them what needs to be done, what medicine to give a patient, whether a patient should be discharged, and so on.
When you’re usually the one in the driver’s seat, having someone tell you to change can bring immediate resistance to change in nursing or healthcare procedures. Some may feel that it’s fine for everyone else to adopt the new way of doing things, but they really don’t have to.
This type of attitude can cause barriers to change in healthcare for other groups because if they see the physicians aren’t changing, they feel they don’t need to either and may ask, “what’s the point?”
Are you looking for more information on questions like: “How will you know if you’re overcoming barriers to change in healthcare?” or “What can I do to effectively be managing resistance to change in healthcare?” Send a message to our change management team.
Why Do Physicians Resist Change?
Why people resist change, including physicians, has to do with the emotions they feel about the change. Finding out what those emotions are is key to moving past these types of barriers to change in healthcare initiatives.
What are some of those emotional reasons that physicians resist changes in healthcare organizations?
They may feel one or more of the following:
- Anxious that the new process will throw them off their daily routine
- Defensive that they have to change at all
- Angry that they’re being told to change when they’re so important to the healthcare process
- Embarrassed that they may not be able to learn the new technology or tool
- Worried that the change will negatively impact patient care
- Frustrated that the new process may take time away from patients (i.e., add to the administrative burden)
- Doubtful the change will work (e.g., “We’ve tried this before and it failed.”)
- Stressed that even more is being asked of them
How To | Changing Physician Culture?
How do you get past all those emotional reasons why people resist change in the physician group? We’ll go over several change management best practices you can use to help get past physician resistance to changes in healthcare organizations.
Explain the Benefits Logically with Data
Physicians tend to be data-driven and spend their time problem solving all day. So, one thing that will help you overcome the barriers to change in healthcare procedures coming from the physician culture is to speak their language.
Show them exactly how the change will benefit the organization, patients, and them and other physicians, and have some data to back that up.
For example, you may express that “hospitals that adopted this same process saw an 80% reduction in administrative errors on patient health records.”
Let Them Know You Respect Their Time
Time is in short supply for most professionals, but it’s especially true for physicians who often have to see as many patients as possible in a day. According to Statista, 33% of primary care physicians spend between 17-24 minutes with each patient, and for 56% of them, it’s even less time.
Come up with training processes that are flexible and can be worked around physician schedules, and that are also time-sensitive. Such as offering some of the training via audio that they could listen to during a commute.
Letting physicians know you’re mindful of their time can help remove some resistance to change in nursing or healthcare projects.
Enlist Key Physicians in Your Organization as Change Agents
Being an outsider coming into the physician culture can make it more difficult not only for you to fully understand why people resist change in that group, but also to have the respect you need to be successful.
When you’re creating your team of change agents and change champions, invite key, well-respected physicians to join in helping communicate about and drive the change.
Other physicians will be more willing to hear what one of their own has to say, and physicians that are change agents will have a better understanding of how to win other physicians over to supporting the changes in healthcare processes you’re making.
Use Your Change Management Toolkit
Once you get past the distinctions between physicians and other groups, you’ll find that many of the core reasons why people resist change come from the same emotional feelings about change.
Just as you do with other groups, use the resistance assessment, communication plan, and other items in your change management toolkit to help find and address resistance to changes in healthcare organizations.
Conclusion: Resolving Barriers to Change in Healthcare
There are many different reasons why people resist change in healthcare organizations, some of them are related to people, and others come from organizations, groups, or technology.
Knowing where barriers to change in healthcare projects come from and how each is unique can help you anticipate them and learn how to resolve each one successfully.
Physicians are a distinct group when it comes to managing changes in healthcare, which can require you to treat them slightly differently to ensure they’re on board with the change and won’t end up causing other groups to give up on the change.
Emotions play a large part in any organizational changes in healthcare processes, so it’s key that whichever change management methodology you use, managing individual transition through change is included as a big part of that.
With the right change management tools and understanding of resistance to change in nursing and healthcare projects, you can manage barriers and help foster support from nurses, physicians, and others for the change initiative.
Read More: Importance of Change Management in an Organization | All You Need to Know
Do you need change management consulting support or help?
Contact Airiodion Group, a specialist change management consultancy that supports organizations, project managers, program leads, transformation leaders, CIOs, COOs, and more, who are navigating complex transformation initiatives. For general questions, contact the OCM Solution team. All content on ocmsolution.com is protected by copyright.
Images: https://stock.adobe.com, Microsoft 365 Clip Art Image(s) (Bing images licensed under the Creative Commons license system.)